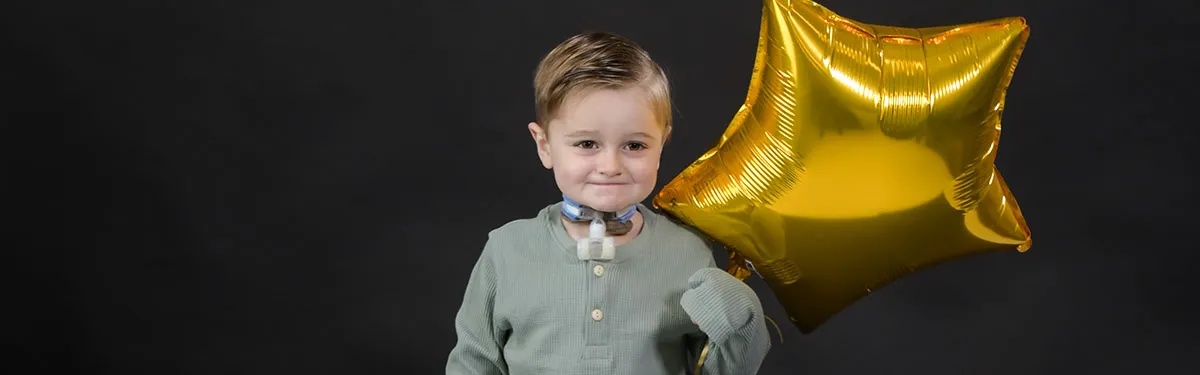
Lincoln
Matt Campbell, M.D., calls Lincoln a miracle kid.
Diagnosed with rhabdomyosarcoma -- a rare type of cancer that forms in soft tissue – then 18-month-old Lincoln had just begun initial rounds of chemotherapy to shrink a golf ball-sized tumor on the back of his tongue when Dr. Campbell, a Pediatric Hematologist/Oncologist at Children’s Health and Assistant Professor at UT Southwestern Medical Center, met him last year.
Lincoln – who already as a toddler has the arm of a baseball pitcher -- had experienced a dramatic entry into Children’s Health, after the tumor was scratched while trying to intubate him for a MRI and put him in cardiac arrest.
He underwent 10 minutes of CPR and had to have an emergency tracheostomy to save his life.
“At that time, we were very hopeful that his tumor was the type that would respond nicely to chemotherapy, and that would make it easier to treat with radiation, which are both treatment options for rhabdomyosarcoma,” Dr. Campbell said. “Unfortunately, after 12 weeks of starting chemotherapy, we found that the tumor had not responded, and it had actually grown through the chemotherapy.”

Dr. Campbell and his fellow physicians had never seen this type of cancer not respond – even if only temporarily – to treatment, and he was worried.
He knew at this point there were few chances for a cure and not many options to offer the family.
“Lincoln is here despite the odds, and it’s incredible,” Dr. Campbell said. “But I have other patients whose cancers come back or don’t respond, and they can’t be removed. In those cases, we really have no options.”
***
The moment when Lincoln’s tumor grew – so big that he couldn’t breathe through his mouth and struggled to breathe through his nose -- was one of the scariest for Lincoln’s parents, Shelly and Chris.
“That was a real punch in the gut,” Chris said. “He’d look up at us, as if he was saying, ‘Help me,’ and we were doing everything we could to fight this.”

After Lincoln’s last dose of radiation – knowing this wasn’t the solution they thought it would be – they took their youngest son home, where he accidentally bit into the tumor and blood filled his tracheostomy tube.
“We were flying in the ambulance to Children’s Medical Center Plano, and I remember my older son asking me, ‘Mommy, is Lincoln going to die?’” Shelly said. “I of course said no, but I honestly didn’t know what the answer was at that point.”
***
One of the only alternatives for Lincoln was surgery to remove the mass from the back of his tongue, but it was risky. The eight-hour operation would involve removing most of his tongue, which would impair his ability to eat and speak.
“Nobody wants to remove something crucial to your child’s life, but we had exhausted most of our options at this point,” Shelly said.
Frustrated by the lack of options for patients like Lincoln, Dr. Campbell has launched a clinical research study for patients with solid tumors that have either not responded appropriately to their first round of therapy or whose cancers have relapsed.
“Compared to about 40 or 50 years ago, we've made a lot of advances in our ability to cure children with cancer,” Dr. Campbell said. “Unfortunately for some children, we have very few, and in some cases, no good treatment options for them. I feel strongly that this is not adequate, and we need to do better.”
Dr. Campbell’s trial will utilize new drugs called immune checkpoint inhibitors, which leans on a discovery that a patient’s immune system can work to fight the cancer and the inhibitor blocks the tumor’s ability to fight back. It’s a medication that has been successful in treating adult cancer patients, but when applied alone, it has not worked in children.
Knowing this, Dr. Campbell will combine these checkpoint inhibitors with chemotherapy to make the tumor more susceptible to the patient’s immune system working to fight off the cancer and handcuff its ability to resist.
“It’s taking care of Lincoln and patients like this that really fuels me to do this research; to have these types of clinical trials; to be able to offer our families something that I really believe can help them,” Dr. Campbell said. “And to be able to offer them some hope.”
The study is supported by donations to Children’s Health, including a grant from Children’s Cancer Fund, which helps fund innovative research studies in the Pauline Allen Gill Center for Cancer and Blood Disorders.
Donations like this are critical to the advancement of the Gill Center to support investments in research so that Children’s Health can continue to offer the best treatment options for patients like Lincoln with cancer and blood disorders.
Earlier this year, Lincoln rang the bell at Children’s Medical Center Plano, signaling the end of his cancer treatment. And for the first time in a long time, his parents breathed a sigh of relief.
“When that day came, it almost didn’t feel real. There were moments when I didn’t know if we would reach this point,” Shelly said. “I thought I was going to be really emotional that day, but instead, I felt at peace.”
Read more patient stories like Lincoln's to learn how Children's Medical Center Foundation impacts the lives of North Texas children.
What to know about pediatric oncology and hematology at Children’s Health
The Pauline Allen Gill Center for Cancer and Blood Disorders at Children’s Health continues to serve as a beacon of hope for children and families within our communities, throughout Texas, and across the country. Not only is the Gill Center a leader in patient care, treatment, research, nursing and staff education, and training in pediatric oncology and hematology, but its affiliation with UT Southwestern and the Harold C. Simmons Cancer Center brings national and international expertise, which sets the Gill Center apart from other sites for pediatric cancer care in the region. From common blood disorders, such as sickle cell anemia, to the rarest forms of cancer, the Gill Center continues to offer comprehensive evaluations, innovative treatments, long-term care, and access to the latest clinical trials.
Last year, the Gill Center served more than 6,000 patients, including nearly 750 new patients; grew the After Cancer Experience program to more than 3,000 pediatric cancer survivors; and saw an increase in sickle cell disease patients, stem cell transplants, and outpatient unit visits.
Patients, like Lincoln, and their families continued to receive incredible psychosocial support through dedicated programs like child life, social work, spiritual care, language interpretation and more, made possible thanks to philanthropic support. Additionally, the Plano campus expansion, which includes an increase in cancer and blood disorder services and specialties to better serve children and families north of Dallas closer to home, continues to see tremendous momentum and support from our community.
Because many of our UTSW physicians actively research and hold leadership positions within the national research community, we are able to study, access, and offer the very best treatment options for cancer and blood disorders. Philanthropy continued to sustain and help grow more than 200 active clinical research trials that help improve the understanding, prevention, diagnosis, or treatment of childhood disease, like next generation tumor sequencing. Five years ago, experts in the Gill Center received pilot funding to begin sequencing next generation tumors from high-risk oncology patients. Today, the program has enrolled and served nearly 400 patients and continues to pave the way to an increase in clinical trials and FDA-approved therapies that target these specific mutations, which can only be identified through the routine use of genetic sequencing.
Philanthropic gifts and resources have been and will continue to be crucial to the advancement of the Gill Center, supporting clinical and research excellence, along with top-notch support programs for our patients and families.
September is National Sickle Cell Awareness Month and Childhood Cancer Awareness Month. Please consider donating in honor of our patients with sickle cell disease and cancer and our team members who care for them every day.
The Gill Center by the numbers in 2021
6,000 patients served
750 new patients
More than 3,000 pediatric cancer survivors served by the After Cancer Experience (ACE) program
200 active clinical research trials that helped improve the understanding, prevention, diagnosis or treatment of childhood diseases
400 patients enrolled in pilot program to sequence next generation tumors from high-risk oncology patients

